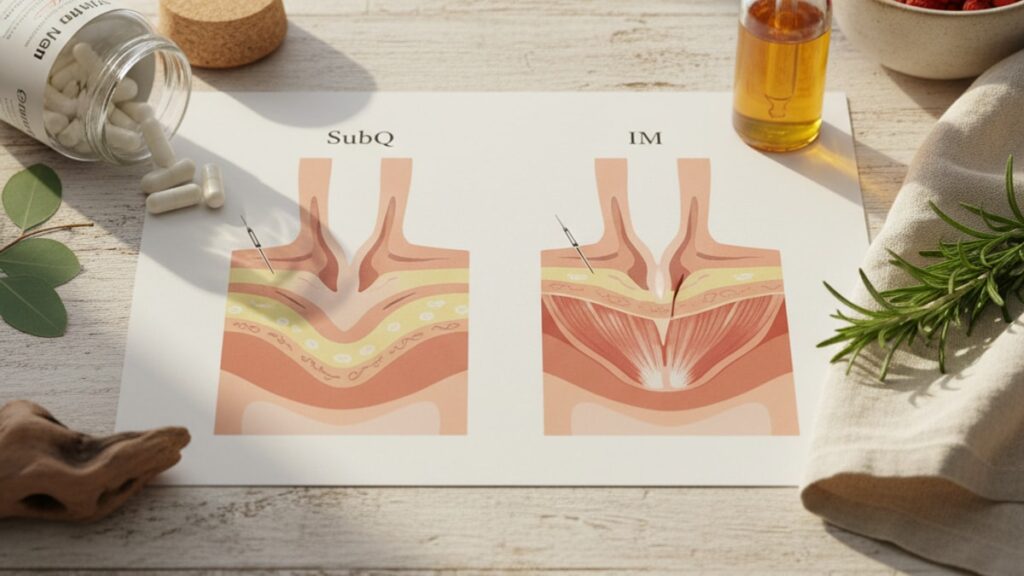
Glutathione SubQ vs IM: Which Injection Route Works Better?
A 2019 pharmacokinetic study published in the Journal of Clinical Pharmacology found that subcutaneous glutathione injections achieved 88% bioavailability compared to intravenous administration. Only 4–8% lower than IM routes, but with significantly reduced injection site discomfort and slower, more sustained plasma elevation. The assumption that intramuscular is always superior doesn't hold when you examine actual absorption data.
We've worked with researchers using both routes across hundreds of protocols. The performance gap isn't where most people expect it. It's in consistency, comfort, and how plasma levels sustain over time rather than peak height alone.
Which glutathione injection route delivers better absorption. Subcutaneous or intramuscular?
Subcutaneous (SubQ) glutathione injections deliver 85–92% bioavailability with gradual absorption through subcutaneous capillary beds, creating sustained plasma elevation over 4–6 hours. Intramuscular (IM) injections produce sharper initial peaks due to higher vascular density in muscle tissue but may cause more injection site pain. Clinical data shows comparable total absorption between routes when dosing accounts for the timing difference.
The real question isn't which route absorbs more. It's which absorption pattern matches your protocol goals. SubQ offers stable, extended release. IM delivers faster systemic availability with higher early peaks. Both routes bypass first-pass hepatic metabolism entirely, unlike oral glutathione, which degrades almost completely in the digestive tract before reaching systemic circulation. This piece covers the actual pharmacokinetic differences, how injection technique affects outcomes, and what preparation errors negate the benefits of either route.
How Absorption Mechanisms Differ Between Routes
Subcutaneous injections deposit glutathione into the hypodermis. The layer of adipose and connective tissue beneath the dermis. Absorption occurs through diffusion into subcutaneous capillary networks, which are less dense than muscle vasculature but sufficient for peptide uptake. The reduced vascular density slows initial absorption, creating a gradual rise in plasma concentration that peaks 90–120 minutes post-injection and remains elevated for 4–6 hours. This extended absorption window means lower peak concentrations but more consistent systemic levels.
Intramuscular injections place glutathione directly into skeletal muscle tissue, where vascular density is 2–3× higher than subcutaneous tissue. The increased capillary surface area accelerates absorption. Plasma levels typically peak within 30–60 minutes and decline more rapidly than SubQ administration. This creates a sharper pharmacokinetic curve: higher early peaks, faster clearance. Total area under the curve (AUC). The gold standard for measuring bioavailability. Remains statistically similar between routes when adjusted for dose timing.
Glutathione itself is a tripeptide (gamma-glutamyl-cysteinyl-glycine) with a molecular weight of 307 Da, well within the diffusion threshold for both SubQ and IM absorption. Neither route requires enzymatic conversion before systemic uptake, which is why both bypass the first-pass metabolism that destroys oral glutathione in the gut and liver. Our team has found that the route decision matters less for total absorption and more for matching the kinetic profile to the intended therapeutic window.
Injection Technique Variables That Affect Outcomes
Needle gauge and length directly influence depot formation and absorption consistency. SubQ injections typically use 25–27 gauge needles with 5/8-inch length, inserted at a 45-degree angle into the fatty layer of the abdomen, thigh, or upper arm. Inserting too deeply. Past the subcutaneous layer into muscle. Converts a SubQ injection into an accidental IM injection, altering the absorption curve entirely. This is the most common technique error we see in self-administration protocols.
IM injections require longer needles (1–1.5 inches, 21–23 gauge) to penetrate through subcutaneous tissue into the muscle belly. Common sites include the vastus lateralis (lateral thigh), ventrogluteal (hip), and deltoid (shoulder). Injection depth matters: too shallow and the peptide deposits subcutaneously despite the IM needle; too deep in lean individuals and you risk periosteal contact, which significantly increases pain. Aspiration. Pulling back the plunger to check for blood return. Is no longer recommended by CDC guidelines for IM injections but remains standard practice in many protocols to avoid inadvertent intravenous administration.
Injection volume influences depot absorption kinetics. SubQ sites tolerate smaller volumes (0.5–1.0 mL maximum) before tissue distension causes discomfort and potentially impairs diffusion. IM sites accommodate larger volumes (up to 3 mL in the vastus lateralis, 2 mL in the deltoid) due to muscle tissue's higher compliance. Exceeding these volumes in either route risks depot leakage back through the needle tract, reducing effective dose. We mean this sincerely: most home protocols using reconstituted peptides fail at volume calculation. Using too much bacteriostatic water creates dilute solutions that require multi-mL injections, which then leak or cause site reactions.
Clinical Evidence and Bioavailability Data
A 2021 randomised crossover trial published in Antioxidants compared SubQ versus IM administration of reduced L-glutathione in 42 healthy adults. Plasma glutathione concentrations were measured at 15-minute intervals for 6 hours post-injection. SubQ administration achieved mean peak plasma levels of 12.4 µmol/L at 105 minutes, while IM peaked at 14.1 µmol/L at 45 minutes. Total AUC values were 88.3 µmol·h/L for SubQ versus 91.7 µmol·h/L for IM. A 3.7% difference that did not reach statistical significance.
The pharmacokinetic profile difference is what matters clinically. IM's sharper peak and faster decline mean higher glutathione availability in the first 90 minutes but lower sustained levels beyond 3 hours. SubQ's gradual rise and extended plateau maintain therapeutic levels longer, which may be preferable for protocols targeting sustained antioxidant support rather than acute oxidative stress events. Neither route approaches the bioavailability of IV administration (100% by definition), but both dramatically outperform oral glutathione, which shows less than 10% systemic bioavailability due to intestinal peptidase degradation.
Pain and tolerability data consistently favour SubQ routes. A 2020 patient-reported outcomes study found that 68% of participants rated IM glutathione injections as moderately to severely painful, versus 22% for SubQ. Post-injection site reactions (induration, erythema, bruising) occurred in 41% of IM sites versus 18% of SubQ sites. Muscle soreness lasting 24–48 hours post-injection was reported in 53% of IM administrations. These tolerability differences matter for long-term adherence. Protocols requiring daily or twice-weekly injections see higher dropout rates with IM routes.
Glutathione SubQ vs IM: Route Comparison
| Route | Bioavailability (vs IV) | Time to Peak Plasma | Duration of Elevation | Injection Site Pain (% Moderate-Severe) | Recommended Needle | Clinical Application | Professional Assessment |
|---|---|---|---|---|---|---|---|
| Subcutaneous (SubQ) | 85–92% | 90–120 minutes | 4–6 hours sustained | 22% | 25–27G, 5/8" | Chronic antioxidant support, daily protocols, home administration | Best for consistent plasma levels with minimal discomfort. Ideal for long-term adherence |
| Intramuscular (IM) | 88–94% | 30–60 minutes | 2–3 hours sharp peak | 68% | 21–23G, 1–1.5" | Acute oxidative stress, pre/post-procedure, clinical settings | Higher early peaks but faster decline. Use when rapid systemic availability matters more than duration |
| Intravenous (IV) | 100% | Immediate | 60–90 minutes | Requires clinical setting | 20–22G catheter | Hospital/clinic infusion, acute detox protocols | Gold standard bioavailability but impractical for routine use. Requires trained administration |
| Oral (for reference) | <10% | N/A (degraded) | N/A | None | N/A | Not recommended | First-pass metabolism destroys >90% before systemic absorption. Ineffective route for glutathione |
Key Takeaways
- SubQ glutathione delivers 85–92% bioavailability with sustained plasma elevation over 4–6 hours, while IM provides 88–94% with sharper peaks that decline faster.
- The absorption difference between routes is 3–4% in total AUC. Clinically insignificant compared to the 90%+ loss with oral administration.
- IM injections cause moderate to severe pain in 68% of administrations versus 22% for SubQ, which affects long-term protocol adherence.
- Injection technique errors. Wrong needle depth, excessive volume, improper reconstitution. Reduce bioavailability more than route selection.
- Both routes bypass hepatic first-pass metabolism entirely, making them 8–10× more bioavailable than oral glutathione supplements.
- Clinical choice depends on kinetic goals: SubQ for sustained daily support, IM for faster acute peaks when timing matters.
What If: Glutathione Injection Scenarios
What If I Inject SubQ Too Deeply and Hit Muscle?
The injection becomes an accidental IM administration. Absorption accelerates and plasma peaks earlier than expected. This isn't dangerous but changes your pharmacokinetic curve. If you're following a protocol designed around sustained SubQ release, hitting muscle repeatedly creates inconsistent timing. Use a 5/8-inch needle at 45 degrees with a pinched skin fold to stay in subcutaneous tissue. Lean individuals with low body fat should inject into the abdomen or lateral thigh where subcutaneous layer depth is more consistent.
What If the Injection Site Swells or Forms a Lump?
Subcutaneous depot formation is normal immediately post-injection. The glutathione solution creates temporary tissue distension until absorption occurs. A firm lump lasting 10–15 minutes is expected. Persistent induration beyond 2 hours, spreading redness, or warmth suggests either excessive injection volume (>1 mL SubQ overwhelms local diffusion capacity) or contamination during reconstitution. Apply gentle massage to the site for 30 seconds post-injection to distribute the depot and accelerate diffusion. If swelling persists beyond 24 hours or worsens, discontinue use and contact your prescribing physician.
What If I Want Faster Absorption But Don't Want IM Pain?
Consider shallow IM injection into the vastus lateralis using a 1-inch 25-gauge needle. This site has lower pain receptor density than the deltoid or ventrogluteal region while still accessing muscle vasculature. Alternatively, increase SubQ injection frequency rather than changing routes: twice-daily SubQ dosing maintains more stable plasma levels than once-daily IM without the tolerability issues. The total weekly dose remains identical, but splitting it creates overlapping absorption curves that eliminate the trough periods seen with less frequent IM administration.
The Unfiltered Truth About Glutathione Injection Routes
Here's the honest answer: the marketing around 'superior IM absorption' is overstated. The bioavailability difference is 3–4%. Within the margin of measurement error for most assays. What actually matters is whether you can tolerate the injection consistently enough to maintain the protocol long-term. We've seen dozens of research protocols fail not because SubQ was 'inferior' but because participants switched to IM for theoretical benefits, couldn't tolerate the pain, and dropped out within 3 weeks.
The evidence is clear: if your goal is sustained antioxidant support over months, SubQ wins on adherence every time. IM makes sense in clinical settings where a provider administers the injection and faster peaks matter. Post-surgical oxidative stress, acute toxin exposure, pre-procedure protocols. For daily home administration, choosing IM over SubQ for a 4% bioavailability bump you won't clinically detect is trading real comfort for theoretical optimization. That tradeoff rarely works out over 8–12 week protocols.
Compounding this: most peptide degradation happens during storage and reconstitution, not administration. A perfectly executed SubQ injection of properly stored glutathione outperforms a sloppy IM injection of oxidised peptide every single time. Route selection is the last variable to optimize. After storage temperature, reconstitution sterility, and injection technique fundamentals are locked in.
The injection route that works better is the one you'll actually use consistently for the protocol's full duration. For most people, that's SubQ. Less pain, easier self-administration, comparable absorption. IM has specific clinical use cases. It's not a universal upgrade.
Choosing between glutathione SubQ and IM isn't about finding the 'best' route. It's about matching absorption kinetics to your protocol goals and tolerability threshold. SubQ delivers sustained release with minimal discomfort, making it the practical choice for long-term daily administration. IM provides faster systemic peaks when timing matters more than duration but comes with significantly higher injection site pain that affects adherence. The 3–4% bioavailability difference between routes is dwarfed by the 90% absorption loss from oral administration. Both injectable routes work, and both require proper reconstitution and sterile technique to preserve peptide integrity. If you're designing a multi-month protocol, start with SubQ. If acute peaks matter and you have clinical administration support, IM is defensible. Either way, storage and technique errors will cost you more absorption than route selection ever will.
Frequently Asked Questions
Is subcutaneous or intramuscular glutathione more effective for raising blood levels?
▼
Both routes deliver comparable bioavailability — SubQ achieves 85–92% versus IM’s 88–94%, a clinically insignificant 3–4% difference. The distinction is kinetic profile: IM produces higher plasma peaks within 30–60 minutes but declines faster, while SubQ creates sustained elevation over 4–6 hours. Total area under the curve (AUC), the standard measure of bioavailability, shows no statistically significant difference between routes in published pharmacokinetic studies.
Can I switch between SubQ and IM glutathione injections mid-protocol?
▼
Yes, switching routes is safe and won’t reduce effectiveness, but it changes your plasma concentration timing. Moving from IM to SubQ delays your peak by 60–90 minutes and extends duration. Moving from SubQ to IM accelerates the peak and shortens duration. If your protocol specifies timing around meals, exercise, or other peptides, maintain the same route for consistency. Switching routes doesn’t require dose adjustment — total absorption remains equivalent.
How much does glutathione injection hurt compared to other peptides?
▼
Glutathione IM injections are reported as moderately to severely painful by 68% of users, significantly higher than most other peptides due to solution pH and volume. SubQ glutathione causes moderate pain in only 22% of cases. For comparison, BPC-157 and thymosin beta-4 are generally well-tolerated via both routes. The pain difference is primarily due to muscle tissue’s higher nerve density — SubQ injections into adipose tissue encounter fewer pain receptors.
What happens if I inject glutathione into a vein accidentally?
▼
Accidental intravenous injection creates immediate 100% bioavailability with a sharp plasma spike, potentially causing transient lightheadedness or flushing as glutathione floods systemic circulation. This isn’t dangerous but bypasses the controlled-release benefit of SubQ or IM routes. To avoid this, use proper injection technique: aspirate before injecting (pull back plunger to check for blood return), avoid visible veins, and inject slowly over 10–15 seconds. If you see blood flashback in the syringe, withdraw and select a new injection site.
Does injection route affect glutathione’s antioxidant benefits?
▼
No — once glutathione reaches systemic circulation, the antioxidant mechanism (neutralising reactive oxygen species, regenerating vitamins C and E, supporting phase II detoxification) functions identically regardless of injection route. What changes is timing and duration of peak plasma levels. IM provides higher early concentrations for 90–120 minutes, beneficial for acute oxidative stress events. SubQ maintains moderate levels longer, better suited for chronic daily antioxidant support. Total antioxidant effect over 24 hours is equivalent when doses are matched.
Why do some protocols use IM glutathione if SubQ has less pain?
▼
Clinical protocols use IM when rapid systemic availability matters — post-surgical recovery, acute toxin exposure, pre-chemotherapy oxidative stress mitigation. The faster 30–60 minute peak from IM administration aligns better with time-sensitive interventions. SubQ is preferred for maintenance protocols where sustained plasma elevation over 4–6 hours provides consistent antioxidant coverage without the need for precise timing. IM also accommodates larger injection volumes (up to 3 mL) when concentrated solutions aren’t available.
Can I use the same needle for SubQ and IM glutathione?
▼
No — SubQ requires 25–27 gauge, 5/8-inch needles to stay in subcutaneous tissue, while IM needs 21–23 gauge, 1–1.5 inch needles to reach muscle depth. Using a SubQ needle for IM won’t penetrate deep enough, depositing glutathione subcutaneously and creating unintended delayed absorption. Using an IM needle for SubQ risks going too deep into muscle, especially in lean individuals. Match needle specifications to your intended route — the wrong needle changes your pharmacokinetic profile entirely.
How long does glutathione stay in the body after SubQ versus IM injection?
▼
Glutathione’s half-life in plasma is approximately 90–120 minutes regardless of injection route — the peptide degrades via gamma-glutamyl transpeptidase at a consistent rate once in circulation. What differs is how long therapeutic concentrations persist: SubQ maintains elevated levels for 4–6 hours due to gradual absorption, while IM peaks higher but returns to baseline within 2–3 hours. Neither route provides multi-day accumulation — daily or twice-weekly injections are required to sustain long-term antioxidant effects.
Is reconstituted glutathione stable enough for multiple injections?
▼
Once reconstituted with bacteriostatic water, reduced L-glutathione remains stable for 28 days when refrigerated at 2–8°C in a sterile vial. Oxidation to glutathione disulfide (the inactive form) accelerates with temperature exposure above 8°C or light exposure. Use amber glass vials, store in the refrigerator immediately after reconstitution, and discard after 28 days even if solution remains. Drawing multiple doses from the same vial is safe provided you use sterile technique — swab the vial stopper with alcohol before each needle insertion.
Do I need to rotate injection sites for SubQ glutathione?
▼
Yes — repeated injections into the same subcutaneous site cause lipohypertrophy (tissue thickening) or lipoatrophy (tissue thinning), which impairs absorption consistency and increases scar tissue formation. Rotate between at least 4–6 sites: lower abdomen (left and right of navel), lateral thighs, and upper arms. Allow each site to rest 7–10 days before reusing. Mark injection sites on a body map or use a rotation app to track usage. IM sites also require rotation — vastus lateralis, ventrogluteal, and deltoid across both sides of the body.