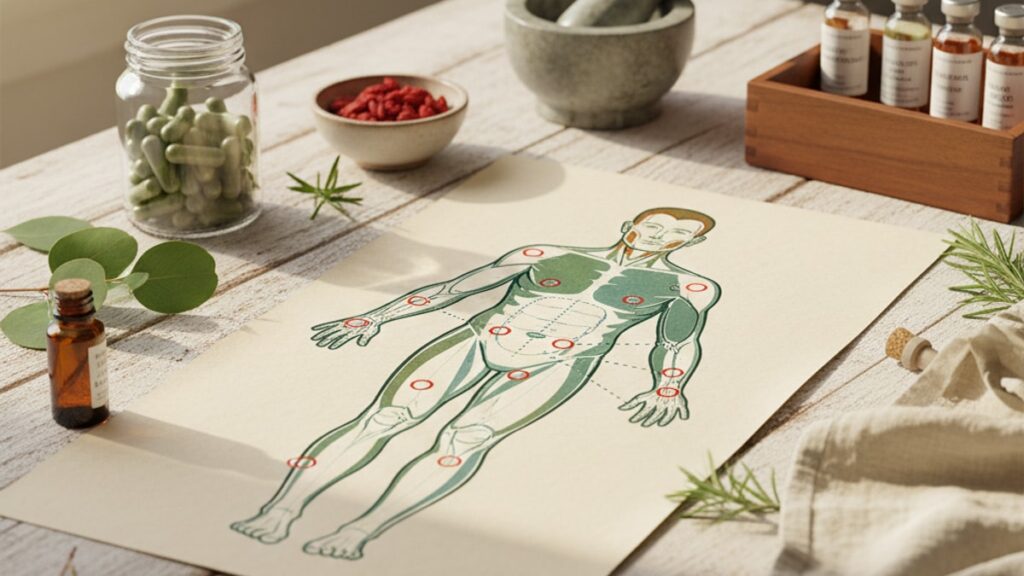
Where to Inject Peptides — Full Body Site Map Guide
A 2023 analysis published in the Journal of Clinical Endocrinology found that subcutaneous injection site choice affects peptide bioavailability by as much as 18%. Yet most home administration protocols provide zero guidance beyond 'inject into fatty tissue.' The difference between optimal absorption and wasted product comes down to three centimetres of anatomical precision. Inject Thymalin into fibrotic tissue from repeated use of the same site, and you've created a depot with unpredictable release kinetics. Inject too shallow, and you're in the dermis. Painful, prone to bruising, and absorbing poorly.
Our team at Real Peptides has guided researchers through peptide reconstitution and administration protocols across hundreds of compounds. The gap between doing it right and doing it wrong isn't technique. It's anatomical knowledge most guides assume you already have.
Where should peptides be injected on the body?
Peptides are injected subcutaneously into fatty tissue 6–12mm beneath the skin surface, with optimal sites including the abdomen (2 inches from the navel), anterior thigh (mid-outer quadrant), and posterior upper arm (triceps region). Site rotation across 8–12 distinct zones prevents lipohypertrophy and maintains consistent absorption. Abdominal sites offer the most predictable pharmacokinetics for growth hormone secretagogues and metabolic peptides due to higher adipocyte density and proximity to portal circulation.
Most injection guides treat all peptides identically. But peptide solubility, half-life, and intended release kinetics vary dramatically. A long-acting GLP-1 analog like semaglutide tolerates slower absorption from adipose-rich sites; a fast-acting nootropic like Dihexa benefits from thinner subcutaneous zones with faster capillary recruitment. What follows maps the five primary injection zones, explains tissue depth targeting for each peptide class, and outlines the rotation protocol that prevents the single most common cause of administration failure. Scar tissue accumulation.
Anatomical Injection Zones: The Five Primary Sites
The abdomen remains the gold standard site for most peptide classes. Not because it's convenient, but because abdominal subcutaneous tissue has the highest adipocyte-to-fibrous-tissue ratio and the most consistent capillary density. Inject 2–3 inches lateral to the umbilicus, avoiding the midline alba (the fibrous band running vertically through the centre). Pinch the tissue. If you can lift a fold of at least 1 inch, you're in viable subcutaneous space. If the tissue feels thin or taut, move laterally. The lower quadrants (below the navel) have slightly higher adipose thickness in most adults, making them ideal for peptides requiring slower, sustained release.
The anterior thigh offers the second-largest injection field. Target the outer mid-thigh, approximately halfway between hip and knee, avoiding the inner thigh entirely (higher nerve density, more painful). Thigh sites work particularly well for peptides dosed daily or multiple times per week because the tissue mass allows 6–8 distinct rotation points per leg. One critical distinction: thigh subcutaneous tissue sits closer to muscle fascia than abdominal tissue does. If you inject too deep or fail to pinch adequately, you risk intramuscular injection. Which changes absorption kinetics entirely and isn't appropriate for most research peptides.
The posterior upper arm (triceps region) provides a compact site suitable for lower-volume injections under 0.5mL. This zone has thinner subcutaneous layers than the abdomen or thigh, making it better suited for peptides that benefit from faster absorption. Short-acting cognitive enhancers or acute metabolic modulators. The disadvantage: it's nearly impossible to self-administer with proper technique using your dominant hand. Most researchers using arm sites require assistance or a mirror setup, which introduces consistency risk.
The upper buttock (dorsogluteal and ventrogluteal zones) offers the deepest subcutaneous tissue reservoir in the body, but it's underutilised in peptide protocols because it requires contortion or assistance to access safely. For researchers rotating through high-frequency protocols (daily injections of CJC1295 Ipamorelin 5MG 5MG blends, for example), buttock sites add 4–6 additional rotation points that significantly delay tissue fatigue. Avoid the lower buttock near the sciatic nerve pathway. Stay in the upper outer quadrant.
The lower back (flanks, just above the iliac crest) represents an often-overlooked fifth zone with moderate adipose thickness and low sensitivity. It's particularly useful for peptides that cause mild injection-site irritation, as flank sites experience less friction from clothing than abdominal sites. The tissue here is slightly more fibrous than abdominal subcutaneous fat, which may marginally slow absorption. Acceptable for depot-style peptides but suboptimal for compounds requiring rapid systemic distribution.
Tissue Depth and Needle Length: Why 6mm Isn't Always Correct
Subcutaneous injection technique assumes a target depth of 6–12mm beneath the skin surface. But that range isn't arbitrary, and it's not universal. Peptide absorption occurs when the injected solution diffuses from the subcutaneous depot into capillary beds within the adipose tissue. Inject too shallow (into the dermis at 2–4mm), and you're in a layer with poor vascular access and high pain-receptor density. Slow absorption, visible welts, and unnecessary discomfort. Inject too deep (past 12mm in lean tissue), and you risk intramuscular placement, which accelerates absorption unpredictably and may denature certain peptides through enzymatic exposure in muscle interstitium.
Needle length must match tissue thickness at the chosen site. A 6mm insulin syringe. The most common format for home peptide administration. Works well for abdominal sites in individuals with BMI above 25, but it may be insufficient for lean individuals injecting into thigh or arm sites, where subcutaneous layers can compress to under 5mm even when pinched. Conversely, an 8mm or 12mm needle in an obese patient with 25mm+ subcutaneous thickness might still land in the correct zone, but it introduces unnecessary depth and higher risk of hitting deeper structures.
The pinch test determines correct needle length: pinch the tissue at your intended site and measure the skinfold thickness with callipers (or estimate visually). If the fold is under 1 inch (25mm), a 6mm needle at a 90-degree angle is appropriate. If the fold exceeds 1.5 inches, you can safely use an 8mm needle. The key is inserting perpendicular to the skin surface after pinching. The pinch lifts subcutaneous fat away from underlying muscle, creating a safe pocket. Inserting at an angle without pinching increases the risk of shallow (dermal) injection.
For peptides requiring intramuscular injection. Rare in research contexts but applicable for certain depot formulations. Target the deltoid (shoulder), vastus lateralis (outer thigh), or ventrogluteal (hip) with a 1-inch (25mm) needle at 90 degrees without pinching. Intramuscular sites are not interchangeable with subcutaneous sites. The absorption profile, peak plasma concentration timing, and enzymatic degradation risk all differ. Unless your protocol explicitly specifies IM administration, default to subcutaneous.
Site Rotation Protocol: The 8-Zone System That Prevents Lipohypertrophy
Repeated injection into the same 2cm² area creates lipohypertrophy. Localised fat overgrowth that forms a fibrotic, poorly vascularised mass. Once lipohypertrophy develops, that site becomes unsuitable for future injections because absorption becomes erratic and incomplete. The condition is cumulative and irreversible without months of site avoidance. The standard rotation protocol for daily or frequent peptide administration uses a minimum 8-zone map, cycling through each site before returning to the first.
Here's the rotation sequence we recommend for subcutaneous peptide protocols: (1) right abdomen upper, (2) left abdomen upper, (3) right abdomen lower, (4) left abdomen lower, (5) right anterior thigh, (6) left anterior thigh, (7) right posterior upper arm, (8) left posterior upper arm. If you inject daily, you return to site 1 on day 9. Sufficient time for micro-trauma healing and capillary bed regeneration. For protocols requiring twice-daily dosing (uncommon but applicable for short-half-life peptides), expand to a 12-zone map by adding right and left flank sites plus right and left upper buttock sites.
Distance matters as much as sequence. Even within a single anatomical zone like 'right abdomen upper,' you should move the injection point at least 1 inch (2.5cm) from the previous injection within that zone. Mark a mental or physical grid: if your last right-abdomen-upper injection was 2 inches right of the navel, place the next one 3 inches right, or 2 inches right and 1 inch superior. This micro-rotation within each zone doubles your effective site count without adding new anatomical areas.
Peptides with longer dosing intervals. Weekly injections of Survodutide Peptide FAT Loss Research or Mazdutide Peptide, for instance. Tolerate simpler 4-zone rotation (right abdomen, left abdomen, right thigh, left thigh) because tissue recovery time between doses is inherently longer. Don't over-rotate low-frequency protocols. It adds complexity without benefit.
Where to Inject Peptides Body Map Site Guide: Side Effect Mitigation by Site
Certain peptides cause predictable injection-site reactions. Localized redness, mild swelling, or transient itching. That vary in intensity depending on site selection. GLP-1 receptor agonists and GIP agonists, including compounds like tirzepatide analogs, are notorious for causing mild inflammatory responses in the first 2–4 weeks of use. These reactions are less pronounced in abdominal sites compared to arm or thigh sites, likely due to differences in subcutaneous immune cell density (mast cells and dendritic cells are more concentrated in limb tissue).
Peptides with higher injection volumes. 0.5mL or above. Cause more discomfort in compact sites like the posterior upper arm. For these, prioritize abdominal or thigh zones where tissue depth accommodates larger depots without stretching the subcutaneous pocket excessively. Injection pain correlates with depot pressure: a 1mL injection into a pinched arm site with 8mm subcutaneous thickness creates significantly higher interstitial pressure than the same volume in a 20mm abdominal fold.
Nootropic peptides and cognitive modulators. Cerebrolysin, P21, and similar compounds. Sometimes cause transient localized tingling or warmth post-injection. This is a vascular response, not an allergic reaction, and it resolves within 10–15 minutes. Anterior thigh sites seem to produce this sensation more frequently than abdominal sites, possibly due to closer proximity to larger nerve bundles. If the sensation bothers you, switch to abdominal rotation exclusively.
Where to Inject Peptides Body Map Site Guide: Peptide-Specific Considerations
| Peptide Class | Optimal Primary Site | Secondary Site | Absorption Considerations | Rotation Frequency |
|---|---|---|---|---|
| Growth hormone secretagogues (MK 677, Hexarelin, Ghrp 2) | Abdomen (2–3 inches lateral to navel) | Anterior thigh | Moderate absorption rate desired; abdominal adipose provides consistent 90–120 min time-to-peak | Daily. 8-zone minimum |
| Metabolic modulators (Tesofensine, Lipo C) | Abdomen or flank | Thigh | Lipotropic compounds benefit from slower release. Deeper adipose preferred | Daily. 8-zone minimum |
| Nootropic and neuroprotective peptides (Cerebrolysin, Dihexa) | Posterior upper arm or thigh | Abdomen | Faster absorption may enhance CNS distribution; thinner subcutaneous layers acceptable | Variable by dosing. 4-zone minimum |
| Immune-modulating peptides (Thymalin, KPV 5MG) | Abdomen or thigh | Flank or upper buttock | Standard subcutaneous absorption; no site-specific advantage documented | Weekly or less. 4-zone sufficient |
| Musculoskeletal support peptides (Cartalax Peptide) | Abdomen or thigh | Flank | Systemic distribution. Site selection based on convenience and rotation needs | Variable by protocol |
| Professional Assessment | For high-frequency protocols (daily or more), abdominal sites offer the largest rotation field and lowest variability. For weekly or less frequent dosing, site choice can prioritize user comfort and accessibility. Rotate between abdomen and thigh as primary zones. Peptides requiring IM administration (rare) are excluded from this table and require deltoid, vastus lateralis, or ventrogluteal targeting with 1-inch needles. |
Key Takeaways
- Subcutaneous peptide injection targets tissue 6–12mm beneath the skin surface. Needle length must match tissue thickness at the chosen site, with 6mm appropriate for most abdominal injections and 8mm safer for lean individuals injecting into thigh or arm.
- Site rotation across a minimum 8-zone map prevents lipohypertrophy, the cumulative fibrotic tissue buildup that renders injection sites unusable and causes erratic absorption.
- Abdominal sites 2–3 inches lateral to the navel provide the most consistent absorption kinetics for growth hormone secretagogues and metabolic peptides due to higher adipocyte density and predictable capillary recruitment.
- Injection-site reactions. Redness, swelling, transient itching. Occur more frequently in limb sites (arms, thighs) compared to abdominal sites due to differences in subcutaneous immune cell distribution.
- Pinching tissue before insertion creates a safe subcutaneous pocket and reduces the risk of intramuscular injection, which alters absorption timing and may expose certain peptides to enzymatic degradation.
- Peptide class influences optimal site selection: fast-acting nootropics benefit from thinner subcutaneous zones with faster capillary access, while depot-style metabolic compounds perform best in deeper adipose tissue.
What If: Peptide Injection Site Scenarios
What If I Hit a Blood Vessel During Injection?
Aspiration (pulling back on the plunger before injecting) is no longer recommended for subcutaneous injections. Modern evidence shows it's unnecessary and increases procedure time without improving safety. If you see blood flashback in the syringe after inserting the needle, withdraw completely, apply pressure to the site with a clean alcohol pad for 30 seconds, and re-inject at a new location at least 1 inch away. Small-vessel puncture during subcutaneous injection is common and clinically insignificant. Capillaries in adipose tissue are numerous and self-sealing. The peptide itself will not be 'lost' into circulation faster; subcutaneous absorption kinetics remain unaffected by minor bleeding.
What If I Accidentally Inject Intramuscularly Instead of Subcutaneously?
Intramuscular injection of a peptide formulated for subcutaneous use accelerates absorption, typically reducing time-to-peak plasma concentration by 30–50%. For most research peptides, this isn't dangerous. It's simply not the intended pharmacokinetic profile. You may notice effects onset faster and dissipate sooner. The bigger risk is repeat IM injection: muscle tissue has higher enzyme activity than adipose tissue, and some peptides (particularly those with specific tertiary structures like SLU PP 332 Peptide) degrade faster in the intramuscular environment. If you suspect IM injection occurred. Common signs include sharper pain on insertion, lack of resistance when depressing the plunger, or post-injection muscle soreness. Switch to a shorter needle and ensure you're pinching tissue adequately before the next dose.
What If I Develop a Hard Lump at an Injection Site?
A firm, non-painful subcutaneous nodule that persists for more than 48 hours after injection indicates either lipohypertrophy from repeated use of that site or an encapsulated depot of undissolved peptide (rare but possible with poorly reconstituted lyophilized peptides). Stop using that site immediately. Mark it off your rotation map for at least 4–6 weeks. The lump will resolve on its own as macrophages clear the depot, but continued injection into fibrotic tissue results in unpredictable absorption and progressive tissue damage. If the lump is red, warm, or increasingly painful, suspect infection or allergic reaction. Discontinue use and consult a medical professional.
What If My Injection Site Bleeds or Bruises After Administration?
Minor bleeding (a droplet of blood at the puncture site) and small bruises (under 1cm diameter) are normal and do not affect peptide absorption. Apply gentle pressure with a clean gauze pad for 60 seconds. Don't rub or massage the site, as this can disperse the peptide depot prematurely. Larger bruises (over 2cm) suggest you've nicked a larger subcutaneous vessel or injected into an area with higher vascular density. For future injections, avoid visible veins on the skin surface and rotate to a different quadrant within your chosen zone. Bruising does not mean the peptide was wasted. Subcutaneous depots remain localized even in the presence of minor hemorrhage.
The Unvarnished Truth About Peptide Injection Sites
Here's the honest answer: most peptide therapy failures aren't caused by the peptide. They're caused by injection-site mismanagement that nobody wants to admit is their fault. Researchers rotating through high-frequency protocols assume site rotation is optional until they develop fibrotic lumps that don't resolve. They ignore pain signals at a particular site because 'it's always been fine' until absorption drops by 20% and they blame compound quality. They use 6mm needles for thigh injections in lean tissue and wonder why they're getting inconsistent effects. You're hitting muscle half the time, and the pharmacokinetic variability is entirely predictable.
The tools for correct administration are cheap, accessible, and well-documented. A $12 set of skinfold calipers tells you which needle length to use. A written rotation log ensures you're not hitting the same 3cm² patch week after week. Alcohol prep pads cost $0.05 each. The failure isn't in the complexity. It's in the assumption that 'inject into fat' is sufficient guidance. It's not. Peptide bioavailability is site-dependent, dose-dependent, and technique-dependent. If you're getting erratic results, audit your injection map before you blame the compound.
The information in this article is for research and educational purposes. Injection site selection, needle length, and rotation protocols should be determined in consultation with qualified research oversight or medical guidance appropriate to your jurisdiction.
How Real Peptides Supports Correct Administration Practices
Every peptide we supply at Real Peptides is accompanied by handling and reconstitution documentation that includes site-selection guidance specific to that compound's solubility and intended kinetics. When you order Thymalin or any other research peptide from our catalogue, you're not just receiving a vial. You're accessing the technical support infrastructure that ensures correct use from reconstitution through administration.
We've worked with research teams across universities and private labs who've reported absorption inconsistencies traced directly to site-selection errors. One recurring case: daily CJC1295 Ipamorelin 5MG 5MG protocols administered exclusively into the same 4cm² abdominal patch for 8 weeks. Predictable lipohypertrophy, unpredictable plasma levels, frustrated researchers convinced the peptide was underdosed. The peptide was fine. The injection map wasn't.
Our commitment to research-grade purity extends to ensuring that purity translates into usable results. You can explore the full range of compounds optimized for diverse research applications in our complete peptide collection. Every product page includes peptide-specific administration considerations and links to third-party certificate-of-analysis documentation. If your research demands consistency, site selection is as critical as compound purity. Both are non-negotiable.
Site rotation isn't bureaucracy. It's the difference between a replicable protocol and guesswork. If you're injecting daily or multiple times per week, map your sites before you start. Not after you've developed scar tissue. The abdomen, thighs, arms, and flanks give you 12+ distinct zones if you use them correctly. Use them.
Frequently Asked Questions
How often should I rotate peptide injection sites?
▼
For daily peptide injections, rotate through a minimum 8-zone map — returning to the first site only after 8 days have passed. This allows sufficient time for micro-trauma healing and prevents lipohypertrophy, the fibrotic tissue buildup that disrupts absorption. For weekly or less frequent protocols, a simpler 4-zone rotation (right abdomen, left abdomen, right thigh, left thigh) is sufficient because tissue recovery time between doses is inherently longer.
Can I inject peptides into my stomach if I have abdominal scarring or loose skin?
▼
Avoid injecting directly into visible scar tissue or areas with significant skin laxity — both conditions reduce subcutaneous vascular density and disrupt absorption kinetics. If you have surgical scars, stay at least 2 inches away from the scar margins. For individuals with loose skin post-weight-loss, pinch the tissue firmly — if you can create a fold of at least 1 inch thickness, the site is viable; if the tissue feels thin or fibrous, switch to anterior thigh or flank sites instead.
What is the correct needle length for subcutaneous peptide injections?
▼
Needle length must match subcutaneous tissue thickness at your chosen site. For abdominal injections in adults with BMI over 25, a 6mm insulin syringe is appropriate. For leaner individuals or thigh/arm injections where tissue compresses to under 10mm when pinched, an 8mm needle ensures reliable subcutaneous placement. Always pinch tissue before inserting and inject at 90 degrees — the pinch lifts adipose away from muscle, creating a safe depot zone.
Does injection site affect how fast peptides work?
▼
Yes — injection site influences absorption rate due to differences in subcutaneous adipose thickness, capillary density, and proximity to larger blood vessels. Abdominal sites provide moderate, consistent absorption with time-to-peak plasma concentration around 90–120 minutes for most peptides. Thinner sites like the posterior upper arm may accelerate absorption by 15–25%, making them preferable for fast-acting compounds. Thigh sites with deeper adipose layers slow absorption slightly, which suits depot-style peptides designed for sustained release.
How much does peptide injection site rotation cost in terms of supplies?
▼
Site rotation itself adds no cost — it’s a technique, not a consumable. The only supply cost is alcohol prep pads (roughly $0.05 per injection) and insulin syringes with appropriate needle length ($0.15–$0.30 per syringe when purchased in bulk boxes of 100). A written rotation log is free. Optional: skinfold calipers for measuring tissue thickness cost $10–$15 and last indefinitely. Total incremental cost for correct site rotation over a year of daily injections is under $150 — negligible compared to the cost of wasted peptides from poor absorption.
Are there injection sites that should be avoided entirely for peptides?
▼
Avoid the following zones: within 2 inches of the umbilicus (navel) — higher nerve density and fibrous tissue; inner thigh — painful due to nerve bundles and offers no advantage over outer thigh; lower buttock near the sciatic nerve; any area with visible veins, active skin infection, or scar tissue. Additionally, never inject into the same 2cm² area more than once per rotation cycle — repeated micro-trauma to identical tissue creates lipohypertrophy that renders the site permanently unsuitable.
What happens if I inject a peptide intramuscularly instead of subcutaneously?
▼
Intramuscular injection accelerates peptide absorption, reducing time-to-peak plasma concentration by 30–50% compared to subcutaneous. For most research peptides, this isn’t dangerous — it’s simply not the intended pharmacokinetic profile, and effects may onset faster but dissipate sooner. The bigger concern is enzymatic degradation: muscle tissue has higher protease activity than adipose, which may partially degrade peptides with complex tertiary structures before systemic absorption. If accidental IM injection occurs, note the timing of effects and switch to a shorter needle with proper pinching technique for subsequent doses.
Can peptides be injected into the same site as insulin or other medications?
▼
No — do not inject peptides into the same anatomical site (within 2 inches) as insulin or other subcutaneous medications on the same day. Co-injecting into overlapping tissue can cause localized depot interactions, unpredictable absorption of both compounds, and increased irritation. If you’re administering multiple subcutaneous medications, assign dedicated anatomical zones to each: for example, use abdominal quadrants exclusively for peptides and rotate insulin to thigh sites only. This ensures independent absorption kinetics and prevents site fatigue from combined injection frequency.
How do I know if I have developed lipohypertrophy from repeated injections?
▼
Lipohypertrophy presents as a firm, raised, non-painful lump in subcutaneous tissue that persists for weeks or months after injection. The tissue feels rubbery or fibrotic compared to surrounding adipose. If you press on the area, it doesn’t indent easily like normal fat. Once lipohypertrophy develops, that site should be avoided entirely for at least 8–12 weeks — continued injection into fibrotic tissue results in erratic absorption and progressive structural damage. Prevention is straightforward: rotate sites methodically and never inject into the same 2cm² area more than once per 8-day cycle.
Is it normal to feel a lump under the skin immediately after injecting a peptide?
▼
Yes — a soft, mobile lump immediately post-injection is normal and represents the peptide depot in subcutaneous tissue. It should dissipate within 15–30 minutes as the solution diffuses into surrounding adipose and enters capillary circulation. If the lump remains firm and palpable for more than 2 hours, you may have injected into an area with insufficient adipose depth or poor vascular access — rotate to a different site for the next dose. If the lump persists beyond 48 hours, becomes painful, or shows redness, discontinue use of that site and monitor for infection.
Should I massage the injection site after administering a peptide?
▼
No — do not massage or rub the injection site after peptide administration. Massaging disperses the subcutaneous depot prematurely and can push the peptide toward deeper tissue layers or into muscle, altering absorption kinetics unpredictably. The only acceptable post-injection action is gentle pressure with a clean gauze pad for 30–60 seconds if minor bleeding occurs. Allow the depot to diffuse naturally through the adipose tissue’s capillary network — this ensures the intended pharmacokinetic profile.
What is the most common mistake researchers make with peptide injection sites?
▼
The most common mistake is failing to rotate sites methodically, leading to lipohypertrophy and erratic absorption within 4–8 weeks of starting a daily protocol. Researchers assume convenience (always injecting in the same spot because ‘it’s easy to reach’) outweighs the biological reality that tissue doesn’t regenerate instantly. The second most common error is using incorrect needle length for tissue thickness — injecting with a 6mm needle into a lean thigh with 7mm subcutaneous depth results in inconsistent depot placement, sometimes subcutaneous and sometimes intramuscular, producing massive variability in plasma levels across doses.